Table of Contents
Bedsores are a common issue for elderly patients.
As people age, movement becomes difficult and limited. The skin begins to thin and sarcopenia causes an age related loss of muscle mass.
Because of this, the elderly are more prone to developing pressure sores.
It can be challenging to manage, especially if you don’t know much about bedsore treatment and prevention.
So today, we will be discussing what bedsores are and how you can manage them better as a caregiver.
Bedsores or pressure ulcers often happen to people with limited mobility.
Also known as pressure sores, these injuries happen to the skin and underlying tissue due to prolonged pressure.
It can affect any part of the body that has consistent pressure, but it is more common in bony areas. These include the heels, elbows, hips, buttocks, and the base of the spine.
Bedsores develop gradually. However, some can take form in just a few hours.
Pressure sores usually occur in the elderly. About 70% of it happens in people over age 65. They are also seen in about 22% of nursing home residents and about 5-23% of hospital patients.

There are three primary contributing factors for bedsores.
First is constant pressure on any part of the body.
Blood flow gets restricted when pressure is applied to an area. This lessens oxygen and nutrient flow, which causes tissue damage.
Friction is also a factor in pressure sores.
The rubbing of the skin on clothing or bedding can cause minor wounds. Moisture in the area can cause the wound to exacerbate, leading to bedsores.
Last but not least is shearing force. Shear is a mechanical force that can cause the skin to tear due to movements in the opposite direction.
Unlike friction sores, shear injury is often seen at the deep tissue level.
These factors may act together to create further damage to the skin. And because seniors often have less movement control, they are more prone to pressure sores.
Other risk factors include immobility and incontinence, especially among seniors.
People with a lack of sensory perceptions like spinal cord injuries and neurological disorders are also at risk.
Medical conditions like diabetes and vascular issues are also more at risk of developing bed sores.
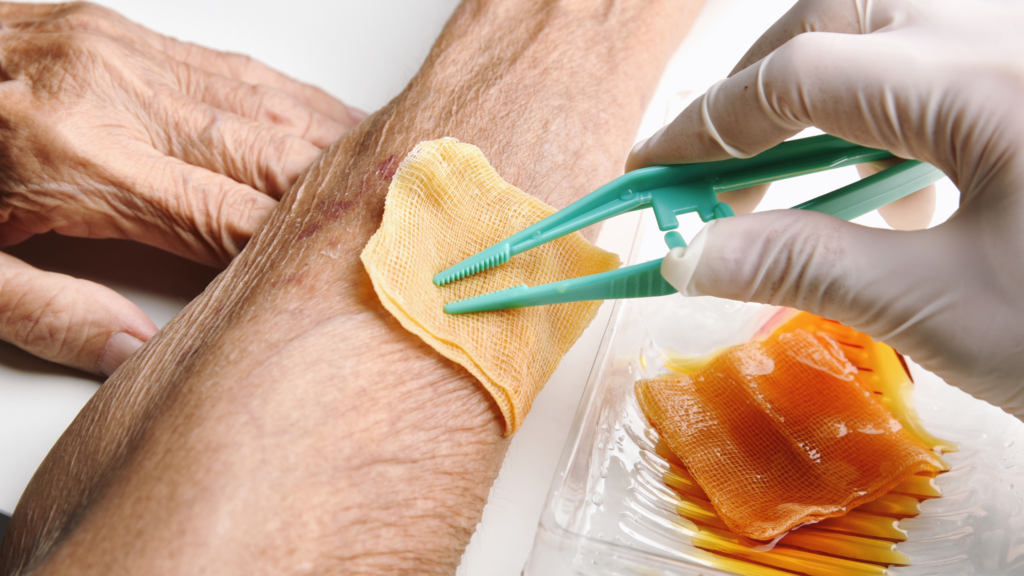
Caregivers can identify bedsores in the elderly by checking on their early symptoms.
Indications include discoloration in the skin. For fair-skinned people, it can show as red patches on the skin. Those with darker complexions can show purple or blue patches.
Pressure sores can also start as patches of skin that feel warm, or spongy. Patients can also complain of pain and itchiness in the affected area.
Doctors and medical professionals may diagnose bedsores according to four stages:
Pressure ulcers that may require debridement usually don’t get better on there own. These wounds have necrotic or infected skin tissue that must be removed to heal.
It reduces infection complications, minimizes scarring, and helps new and healthy tissue growth.
Learn more about debridement here.
The leading cause of pressure ulcers among seniors is the lack of movement.
Seniors who are no longer able to age in place turn to nursing homes for care.
Ideally, the staff in these homes should meet the requirements of the residents to prevent sores.
Such as proper positioning to reduce weight through bony prominences and changing the position every 2 hours.
However, the leading cause of bedsores among seniors is neglect.
If they can’t shift their weight or have issues with movement, bedsores will eventually develop.
Seniors who are in the later stages of Alzheimer’s disease or dementia often experience this too.

This is why primary caregivers should know why pressure sores happen. It is also necessary to take the proper steps to prevent them.
What happens if you ignore the early symptoms of bedsores? It can be catastrophic.
While rare, untreated pressure sores can lead to carcinoma, a type of cancer that affects the internal or external lining of the body.
It can also lead to bone and joint infections, eventually leading to long-term damage to tissues and cartilage.
Untreated infections can also lead to sepsis and even death.
Although bedsores in the elderly may seem like a minor issue, they can quickly become more severe and eventually lead to death if not treated properly.
Caregivers should be aware of the early signs of bedsores in order to avoid any further complications.
In my next blog post, I’ll be sharing tips on how you could prevent bedsores in seniors, so be on the lookout!
That's all for today.
Take care, keep mom safe and have a great day!
Winn