Table of Contents
Musculoskeletal disorders are common in the elderly.
According to WHO, approximately 1.71 billion people suffer from musculoskeletal disorders worldwide.
Lower back pain is the most common and is the single leading cause of disability in 160 countries.
Most of these numbers are in the elderly. And as the population grows older, it is projected to increase in the next decades.
So today, I am sharing five common musculoskeletal disorders and how you can manage them better.

Our bodies can become weaker with age. That includes our muscles, bones, and joints.
Most of the time, our joints are affected by the changes that happen in the cartilage and other connective tissues.
Aging causes our bodies to produce fewer proteoglycans, a substance that keeps the cartilage resilient. Because of this, the surface of the joints becomes less lubricated.
The joints become stiffer and the tendons and ligaments also become rigid and brittle.
This limits the joint’s range of motion and can eventually lead to osteoarthritis.
We also experience muscle loss starting at the age of 30. This condition is called sarcopenia.
As we age, the amount of muscle tissue and fibers decreases gradually. This results in additional strain to specific joints, causing us to lose balance and even be more at risk for falls.
Certain conditions also affect the impairment of musculoskeletal functions. Diseases like diabetes, metabolic syndrome, chronic kidney disease, and stroke are also associated with skeletal dysfunctions in the elderly.
Read more about the effects of aging on muscle function here.
It can be challenging for caregivers to identify musculoskeletal disorders in seniors.
Most of the time, elderly people dismiss pain and body ache as part of aging. And more often, our aging parents would self-medicate instead of getting the right treatment.
The problem is, untreated pain can be chronic. It can also heavily affect their quality of life.
Chronic pain is defined as any pain that doesn’t go away in at least three months. And it’s also possible that these are early signs of musculoskeletal disorders.
Here are some of the most common disorders in muscles, joints, and bones in the elderly.
Low back pain can be a combination of symptoms. It can range from mild to severe and debilitating.
Some of the symptoms can feel like a dull pain that is contained to the lower back.
It can also be a stinging, burning pain that moves from the back of the thighs and lower leg or feet. Sometimes it can be accompanied by numbness or tingling as well.
Muscle spasms can also be a symptom, including tightness in the lower back, pelvic area, and hips.
Lower back pain is usually described by type and duration.
Acute pain typically comes suddenly and can last for a few days. It can indicate the body’s usual response to injury or tissue damage. The pain also lessens as the body heals.
If it lasts about six weeks to three months, it can be categorized as subacute low back pain. This might be caused by prolonged muscle strain or joint pain. This case may need medical assistance if it affects daily activities.
Chronic back pain is usually defined if it lasts more than three months. It is usually severe and doesn’t respond to initial treatment. It also needs a thorough medical workup to identify the source of the pain.
Two common types of back pain are axial and radicular pain.
Axial pain is primarily from muscles, ligaments, joints, or bones in and around the spine. The pain tends to be localized to the lower back, butt, and the top of the legs.
Radicular pain, on the other hand, occurs if a spinal nerve root becomes inflamed. This causes a sharp, electric, burning type of pain.
It is usually felt on only one side of the body and is associated with numbness or weakness.
Elderly-onset rheumatoid arthritis happens between 60-65 years old. However, some get arthritis as early as 30 years old.
It usually affects large joints like the shoulders. It is also usually less severe unless you also have a rheumatoid factor.
Symptoms can include fever, myalgia, weight loss, and anemia. It can also overlap with other diseases like osteoarthritis, rotator cuff tendinitis, hypothyroidism, and Parkinson’s disease.
Elderly people with rheumatoid arthritis often experience stiffness in the morning along with warm, tender, and swollen joints.

Geriatric fractures often happen due to falls, trauma, or a direct blow to the body. It can also be caused by overuse or repetitive motions.
Common symptoms of a fracture may include sudden pain, swelling, and trouble in moving the injured area or nearby joints.
Frozen shoulders or adhesive capsulitis is a condition where there is stiffness in your joints and shoulders.
The chances of developing frozen shoulders can increase if you’re recovering from a medical procedure that limits arm movement.
Frozen shoulders typically develop in three stages. In the freezing stage, shoulder movement can cause pain and limit movement.
The frozen stage can make the shoulder stiffer despite the pain diminishing. In the thawing stage, the shoulder movement and range begin to improve.
According to WHO, falls are the second leading cause of unintentional injury and deaths in the world.
It is estimated that 684,000 individuals die from falls. And adults older than 60 years old suffer the most fatal ones.
In the US alone, 20-30% of the elderly who suffer from falls encounter moderate to severe injuries. These can include hip fractures or head trauma.
A huge part of it has to do with the physical and cognitive changes that come with aging. And most accidents have to do with environments that are not adapted for an aging population.
Read more about how to prevent fall-related injuries in the elderly here.
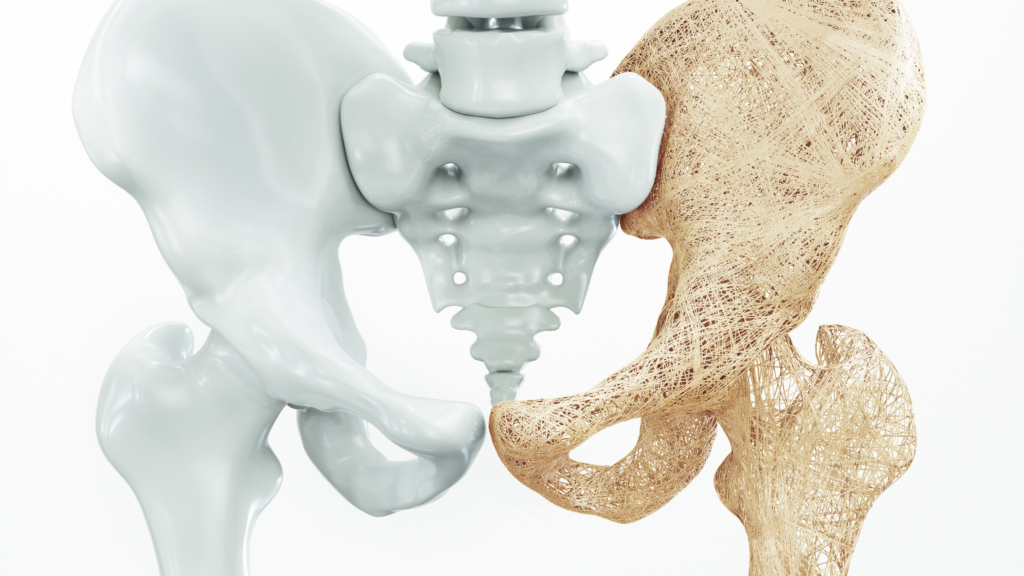
Osteoporosis is a condition that causes the bones to become weak and brittle. It occurs when the body can’t create new bones to replace weak, damaged ones.
Osteoporosis can affect both men and women. Unfortunately, Asian and Caucasian women who are past menopause are more prone to it.
Low calcium intake has a huge impact on bone density. Those with eating disorders and gastrointestinal surgery can also affect bone health.
Long-term use of corticosteroid medications can also interfere with the bone rebuilding process. It is also associated with medications related to seizures, cancer, gastric reflux, and transplant rejection.
Those with Celiac disease, kidney or liver disease, and rheumatoid arthritis also have a higher chance of developing osteoporosis.
Bad habits and lifestyle choices can also lead to weakened bones, like having a sedentary lifestyle, excessive alcohol and tobacco use.
Learn more about osteoporosis here.

Degenerative disc disease can happen in any area of the spine. It’s a condition where the spinal discs lose their flexibility and height to cushion the spine.
Because discs have limited blood supplies, it can be difficult for them to repair themselves.
As we grow older, the discs dry out and shrink. It slowly loses water and flexibility, putting more stress on the disc annulus.
Sometimes the nucleus pushes through a tear in the annulus wall and causes inflammation in the nearby nerves.
Bone spurs can also grow in between the vertebrae leading to disc degeneration.
Learn more about degenerative disc disease here.
There are many ways to manage musculoskeletal disorders in seniors. And most of them are simple and doable.
First, we need to learn how to manage our loved one’s weight.
Being overweight can be a huge contributor to joint pressure and pain. The more pounds they have, the more it strains the body.
Start with managing your elder’s diet better. Give more fiber-rich food to keep them full and their digestion better.

Read more about how to prevent digestion problems in seniors here.
Limit sweets and sugary drinks as they can boost inflammation and increase the chances of arthritis.
Keep them hydrated by giving them small drinks every hour. Our bodies require lots of fluids to maintain lubrication so make sure to offer water regularly.
It’s also best for you to keep our elderly moving. Instead of strenuous activities like running, go for low-impact exercises like walking and swimming.
You can also encourage them to do resistance training indoors with stretch bands.
Work on their core muscles to strengthen them to help them avoid fall-related injuries.

It is also best to talk to experts and physical therapists to help with the right guides before engaging in any exercise.
And if any chronic pain occurs, always go to your doctor before offering any medications and treatments.
Musculoskeletal disorders and problems are common in seniors. But it doesn’t mean they should suffer in silence.
The key is to make sure they’re getting the help they need.
Talk to your doctor. Make sure they have a senior-friendly environment. And keep them healthy and on the move.
Need help with making your aging parent’s place safer? Send me a message for a free consultation.
That’s all for today.
Take care, keep mom safe and have a great day!
Winn